Patella Apophysitis | Sinding-Larsen-Johansson (SLJ) Syndrome
Patella apophysitis, or Sinding-Larsen-Johansson (SLJ) syndrome as it’s still widely known, is a common cause of knee pain in children. While it can be concerning to see your child in pain or unable to participate in activities that they enjoy, this condition typically responds very well to appropriate management.
In this blog, we explain what patella apophysitis is, what causes it, how it is diagnosed and how physiotherapy can help your child successfully return to sport. You can read more about other common causes of knee pain in children here.
What is patella apophysitis?
Patella apophysitis — commonly referred to as Sinding-Larsen-Johansson (SLJ) syndrome — refers to irritation of the growth plate at the bottom of the kneecap (patella). It typically affects children aged 10–14 years during growth spurts, particularly those involved in jumping and sprinting sports such as football, gymnastics and athletics.
The condition occurs where the patellar tendon attaches to the bottom of the kneecap. During periods of skeletal immaturity, this area is more vulnerable to repetitive stress.
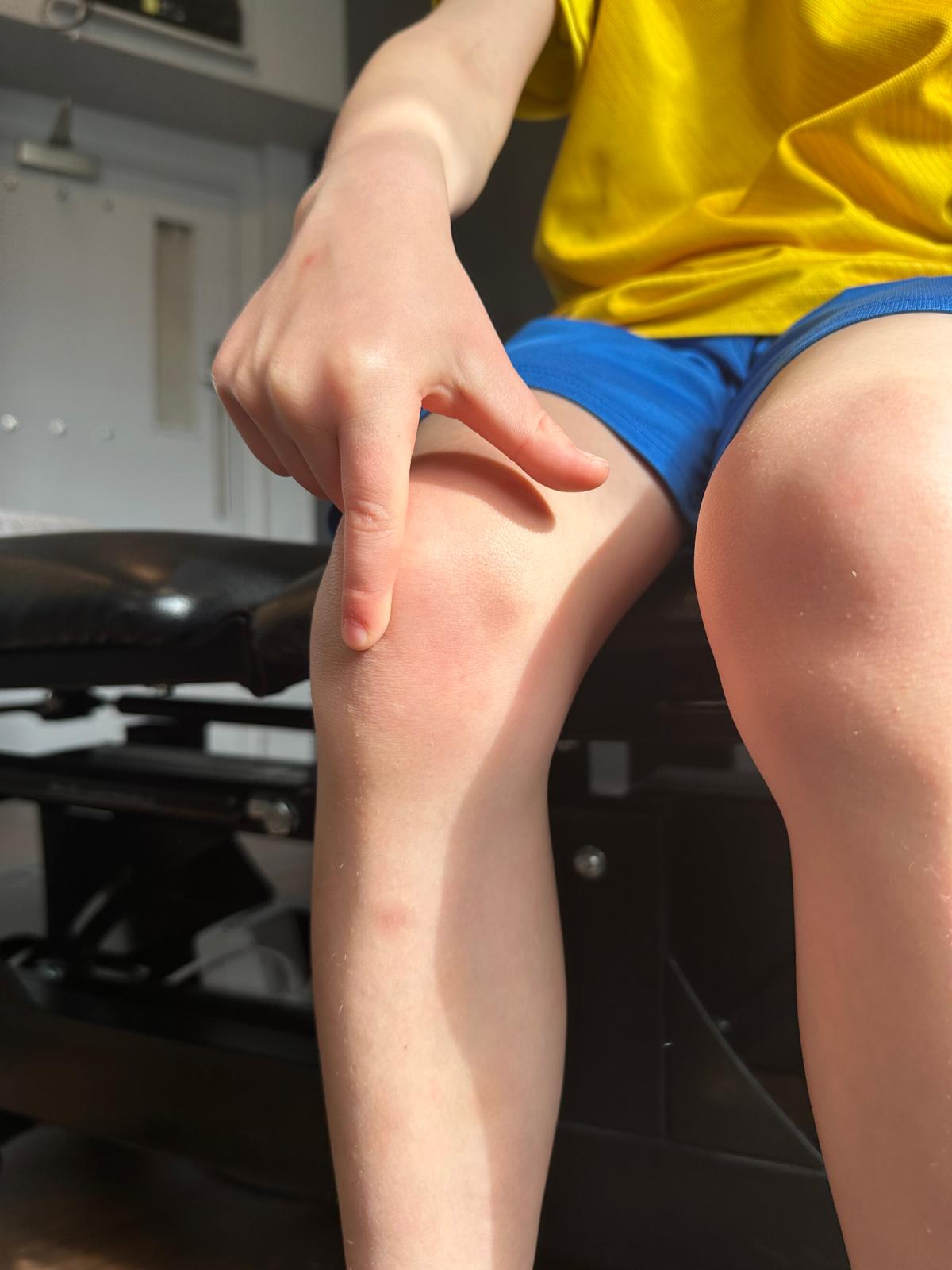
Symptoms include:
- Localised pain at the bottom of the kneecap
- Tenderness when pressing the affected area
- Pain during running, jumping and squatting
- Pain after activity that improves with rest
Patella apophysitis is considered self-limiting, meaning symptoms typically resolve once skeletal maturity is reached and the growth plate closes. However, without proper load management and rehabilitation, symptoms can persist and limit participation in sport.
What causes it?
Patella apophysitis is a traction apophysitis — meaning it develops from repetitive pulling forces through the patellar tendon onto the immature bone.
Contributing factors include:
- Rapid growth: Bones lengthen quickly during adolescence, often before the muscles can adapt, increasing tension across the knee
- Repetitive jumping and sprinting: High-load activities increase strain on the growth plate
- Quadriceps tightness: Reduced flexibility in the muscles at the front of the thigh can increase traction forces through the patellar tendon
- Training load errors: Sudden increases in frequency, intensity or duration of sport can overload the developing knee.
Patella apophysitis is closely related to other growth-related traction injuries such as tibial apophysitis (Osgood-Schlatter disease), but the key difference is location — patella apophysitis affects the lower pole of the patella, whereas Osgood-Schlatter affects the tibial tuberosity.
How is patella apophysitis diagnosed?
Diagnosis is made clinically through:
- A detailed history of growth and activity levels
- Localised tenderness at the inferior pole of the patella
- Pain reproduced with resisted knee extension or jumping
- Assessment of quadriceps strength and flexibility
Imaging is not routinely required unless symptoms are severe or atypical. In some cases, ultrasound or X-ray may show changes at the lower patella, but clinical examination is usually sufficient to make a diagnosis of patella apophysitis.
How is it treated?
Evidence supports exercise-based rehabilitation and load modification as the primary management strategies for traction apophysitis. Management is conservative and highly effective when addressed early.
Treatment typically includes:
- Activity modification: Temporarily reducing high-impact and jumping activities while maintaining general fitness.
- Load management planning: Structured return to sport based on symptom response.
- Targeted strengthening: Progressive strengthening of the quadriceps, hip musculature and lower limb kinetic chain to improve load tolerance.
- Flexibility work: Addressing quadriceps tightness to reduce traction stress.
- Education: Supporting children and parents in understanding growth-related conditions and preventing recurrence.

Crucially, children with knee pain should be assessed and treated by a physiotherapist who has undergone specialist training in paediatrics.
Growth-related knee conditions require expertise in skeletal development, age-appropriate rehabilitation and safe progression back to sport. A physiotherapist with paediatric training can design a personalised programme tailored to your child’s growth stage and sporting demands which can can significantly shorten recovery time and prevent recurrence.
With the right management, most children return to full sport participation without long-term problems.
Help your child get back to sport — pain free!
If your child is experiencing knee pain that’s interfering with activity, we’re here to help. Contact our friendly reception team on 0114 2678181 to book an assessment with one of our paediatric physiotherapy specialists.






