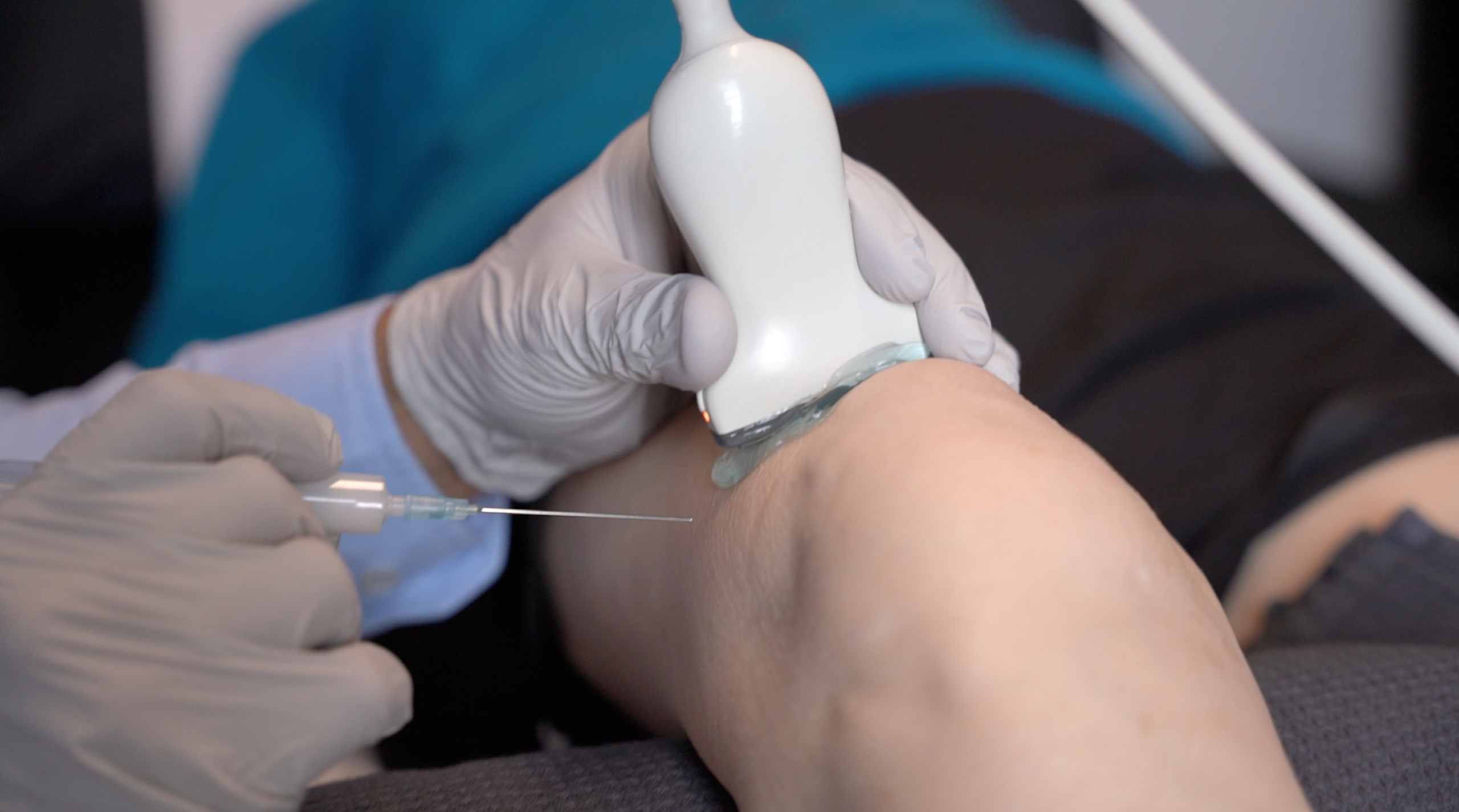
Injection Therapy FAQ’s
Here are some common Injection Therapy FAQ’s if you are considering a cortisone, Hyaluronic acid or a combined injection here at The Physios. There is lots more information regarding injections here. If you can’t find what you are looking for, simple get in touch and we will get back to you as soon as we can.
What precautions do I need to take if I am taking blood thinning medication?
It depends on the type of medication you are on and the area that is being injected. Most people are now on anti-platelet drugs such as Aspirin or Clopidogrel or NOACs such as Apixaban and Rivaroxaban. Because these drugs don’t stay in your system for longer than a few hours, it is usually safe to miss the dose immediately before the injection and resume the dose afterwards. For example, if you take Apixaban once daily in the morning and your injection appointment is during the day, you would miss the dose on the day of the injection and resume your medication the following morning. This may not always be the case and it is therefore essential that you discuss this with your physiotherapist prior to your injection appointment.
If you are taking anti-coagulant drugs such as Warfarin, you will need to know your INR value which needs to be 2.4 or lower before injection treatment can be considered. In some cases discontinuing your Warfarin for a short period of time may be necessary but this MUST ONLY be done in consultation with your doctor.
What are the possible side effects to a Cortisone injection?
Side effects from a steroid injection are very rare. Your safety is of paramount importance and great care is taken to ensure any risks are minimised.
Infection is the most serious side effect although its incidence has been estimated to be in the region of 1:40,000. Whilst extremely rare, everyone is warned that increasing pain, redness, heat, swelling around the injection site and feeling unwell could be signs of an infection and immediate medical assistance is warranted.
Allergic reaction (including anaphylaxis) is another rarity but with increasing incidents reported in the media every care is taken to avoid this. Local anaesthetic has been known to trigger an allergic response and we tend to avoid using this where possible.
Local skin changes can occur where the skin gets lighter (depigmentation) and the skin contours diminish slightly (sub-cutaneous atrophy) but these are usually temporary and recover over several months.
Tendon damage has been reported where tendons are repeatedly exposed to steroid injections and this practice is avoided.
Pain ‘flares’ are occasional reported in the first 24 hours after injection although this again is unusual. Simple paracetamol will settle any discomfort.
What are the possible side effects to a Hyaluronic Acid (HA) injection?
None of the side effects of cortisone injections really apply to HA injections apart from the remote chance of infection. This is further reduced with HA because it does not share the immunosuppressive properties that steroids like cortisone have. Side effects from HA therefore are very rarely experienced which provides part of the attraction to their use in clinical practice.
What are the possible side effects to a PRP or cellular matrix injection?
As with HA injections, there is a remote chance of infection. Platelet rich plasma or cellular matrix injections do require a small amount of blood to be taken from the front of the arm (in much the same way as giving blood). It is also common to experience some discomfort following the injection.
Can I drive after the injection?
That largely depends on you! There are no medical reasons why you shouldn’t drive after the injection (we usually monitor you for around 30 mins after the injection) but some people prefer to arrange to come with someone so they don’t have to drive home.
Should I rest after the injection?
If you have an injection into a joint, you should rest it, or at least avoid strenuous exercise, for the first 1–2 days. It’s also important, however, not to rest for too long. We recommend that you return to your physiotherapist within 5-7 days of the injection to check the outcome of the injection and to resume your rehabilitation.
Will I need more than one injection?
With cortisone and hyaluronic acid injections, your usually only require one injection. However, if you have a long-standing condition you may well benefit from repeated injections, provided there is an interval of several months between each one. In specific cases, it may be necessary to inject more frequently (e.g. Frozen shoulder).
With PRP and cellular matrix injections, the scientific literature and our specific protocol requires a series of 3 injections at monthly intervals.